In contemporary society, the acceleration of lifestyle pace and changes in dietary habits have made fatty liver disease a common liver condition. Unlike colds or fevers that come with obvious discomforts, fatty liver disease silently invades our health.
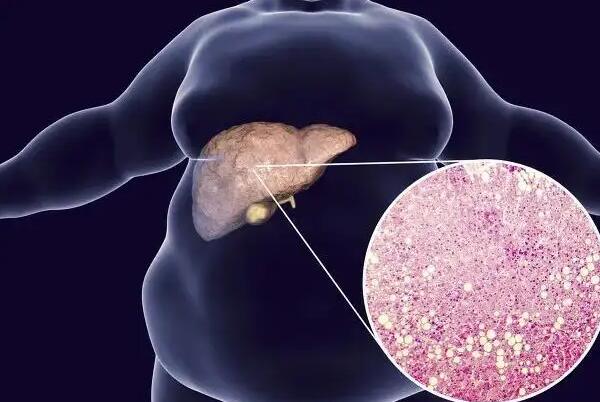
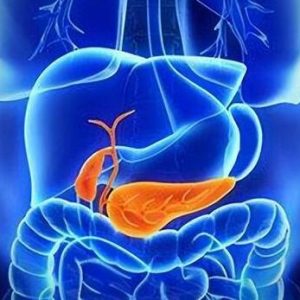
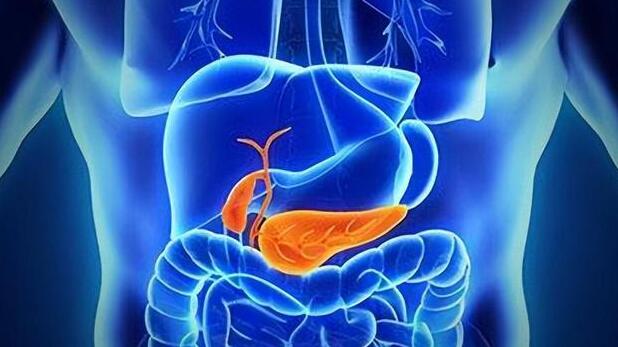
Fatty liver disease, also known as hepatic steatosis, is a condition characterized by an excessive accumulation of fat within liver cells. This pathological state isn’t an independent disease but rather a liver alteration caused by various factors. Normally, liver cells contain no fat or just trace amounts. When the fat content in liver cells exceeds 5%, it’s classified as fatty liver disease.
Depending on the level of fat content, fatty liver can be categorized into mild (5%-10%), moderate (10%-25%), and severe (>25%).
Types of Fatty Liver
There are two main types of fatty liver disease:
1. Non-alcoholic fatty liver disease (NAFLD): This is the most common type, unrelated to alcohol consumption. It’s often associated with metabolic syndrome, which includes obesity, hypertension, diabetes, and dyslipidemia. NAFLD can further be divided into two subtypes:
Non-alcoholic fatty liver (NAFL): A milder form where the liver has excess fat but no inflammation or damage.
Non-alcoholic steatohepatitis (NASH): A more severe form where high fat levels in the liver are accompanied by inflammation and liver cell damage. Prolonged inflammation may lead to fibrosis and even cirrhosis.
2. Alcoholic fatty liver disease (AFLD): As the name suggests, AFLD is closely linked to long-term excessive alcohol consumption. Excessive alcohol disrupts normal fat metabolism, leading to fat accumulation in the liver. AFLD can progress to alcoholic hepatitis and cirrhosis.
For any type of fatty liver disease, early diagnosis and lifestyle changes are key to preventing its progression.
The Dangers of Fatty Liver
Although early-stage fatty liver might be asymptomatic, neglecting it could lead to serious liver conditions like hepatitis, fibrosis, cirrhosis, and even liver cancer. These advanced liver diseases are not only difficult to treat but also significantly impact quality of life.
How Does a Healthy Liver Turn into a Fatty Liver?
A fatty liver develops when there’s an excess accumulation of fat in the liver without overconsuming alcohol. Here are some potential causes:
1. Dietary habits: High-sugar, high-fat, high-calorie diets can promote fat buildup in the liver.
2. Obesity: Being overweight or obese is a major risk factor for developing fatty liver disease.
3. Diabetes and insulin resistance: These metabolic disorders can lead to abnormal fat metabolism and increased risk of fat accumulation in the liver.
4. Dyslipidemia: High cholesterol and triglyceride levels in the blood are closely related to fatty liver development.
5. Lack of exercise: Physical inactivity can cause fat storage and increase the risk of fatty liver.
6. Certain medications: Drugs like corticosteroids, estrogens, some antivirals, and chemotherapy drugs may increase the risk of fatty liver.
7. Rapid weight loss: Extreme or very rapid weight reduction can sometimes lead to fatty liver.
8. Genetic factors: Family history can be a contributing factor, with some individuals predisposed to the condition.
9. Other health conditions: Conditions like hepatitis and autoimmune liver diseases may also play a role in fatty liver development.
When your liver contains more than 5% fat relative to its normal weight, doctors may diagnose fatty liver disease. If left untreated, it can progress to hepatitis, cirrhosis, or even liver cancer.
Diagnosing Fatty Liver
1. Physical examination: Doctors may find an enlarged liver through palpation, though this method isn’t precise for early or mild cases.
2. Blood tests: Elevated levels of enzymes like ALT and AST indicate liver dysfunction but aren’t specific to fatty liver as they can rise in other liver conditions.
3. Ultrasound: The most common non-invasive tool for detecting fatty liver, ultrasound imaging shows fat deposits in the liver.
4. CT scans: Provide more detailed images than ultrasound, helping assess the severity of fatty liver. However, radiation exposure usually makes it a less preferred option.
5. MRI: Offers detailed information about fat distribution without radiation risks but is costlier, so it’s not typically used for initial screening.
6. Liver biopsy: Despite being invasive, a liver biopsy is the gold standard for determining the extent of fatty liver and whether there’s inflammation or fibrosis. It may be performed when other tests are inconclusive or require further evaluation.
Prevention and Early Detection Tips:
1. Fatty liver may be asymptomatic in early stages, sometimes discovered incidentally during check-ups.
2. If you have metabolic syndrome factors like obesity, diabetes, or dyslipidemia, regular liver function tests and ultrasounds are recommended.
3. With a family history or other risk factors, stay vigilant with regular screenings.
For non-alcoholic fatty liver, controlling blood sugar and lipid levels is crucial. If NASH or significant fibrosis has developed, treatment may require personalized approaches, including medication.
Treating Fatty Liver
1. Weight loss and healthy diet: Gradually losing weight, aiming for a 10% reduction, can significantly reduce liver fat content.
Increase fruit and vegetable intake and cut down on high-fat, high-sugar foods.
Consider the Mediterranean diet rich in whole grains, healthy fats (like olive oil), and quality proteins.
2. Regular exercise: Engage in aerobic and strength training activities, such as brisk walking, swimming, or cycling.
At least 150 minutes of moderate-intensity exercise per week is recommended for maintaining health.
3. Manage related health issues: Actively control conditions like diabetes, hypertension, or high cholesterol.
Work with your doctor to adjust medications to improve metabolic indicators.
4. Limit alcohol intake: Even if not the cause of fatty liver, avoiding or limiting alcohol is vital as it can worsen liver damage.
5. Avoid harmful substances: Steer clear of unnecessary medications and substances potentially toxic to the liver.
6. Review medications: Some drugs can cause or exacerbate fatty liver; discuss current medications and supplements with your doctor to see if adjustments are needed.
7. Monitoring and regular assessment: Regular liver function tests and ultrasounds to monitor the liver’s condition and evaluate treatment effectiveness.
8. Medication: No specific drugs are approved for fatty liver disease, but for conditions like NASH or fibrosis, specific medications—such as anti-inflammatory drugs, antioxidants, and insulin sensitizers—may be considered.
9. Surgery: For severely obese patients unable to change their lifestyle, weight loss surgery may be considered.
The final treatment plan should be tailored by a healthcare professional based on individual circumstances. Following up closely with your doctor and undergoing necessary regular checks is essential.
Daily Life Considerations for Managing Fatty Liver
1. Balanced diet:
Maintain a balanced diet with low-sugar, high-fiber foods like whole grains, fruits, and vegetables.
Control fat intake, especially saturated and trans fats.
Reduce rapidly digestible carbohydrates like white rice and bread.
2. Avoid alcohol: Even if not diagnosed with alcoholic liver disease, limit or completely abstain from alcohol.
3. Regular exercise: Establish a consistent exercise routine to help manage weight and reduce liver fat.
Combine aerobic and strength training to boost metabolism.
4. Maintain a healthy weight: Seek professional guidance for weight management if overweight or obese.
5. Monitor blood sugar: Control blood sugar levels if you’re diabetic by following dietary and medication guidelines set by your doctor.
6. Manage cholesterol: Regularly check cholesterol levels and control them through diet, exercise, and medication if needed.
7. Avoid hepatotoxic drugs: Consult a healthcare provider before using over-the-counter drugs, prescription drugs, or supplements to avoid additional strain on the liver.
8. Regular check-ups: Regularly perform liver function tests and other relevant examinations to monitor disease progression and treatment effects.
9. Stress management: Practice stress relief techniques like meditation, yoga, or deep breathing to reduce stress impacts on health.
10. Good sleep: Adequate sleep aids in recovery and metabolism regulation.
11. Quit smoking: Smoking may accelerate liver disease progression; quitting is beneficial for overall health.
Each change should be made under medical guidance to ensure they suit your specific health needs.
Fatty liver isn’t just a “disease of the wealthy”; anyone can encounter it. Cultivating healthy habits, focusing on diet and exercise, maintaining regular check-ups—all are effective strategies against fatty liver disease.