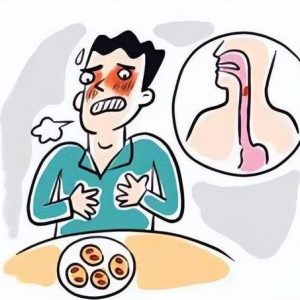
Deep within the acidic fortress of human stomachs lies a microbial survivor: Helicobacter pylori, a spiral-shaped, microaerophilic, Gram-negative bacterium. This unique organism is the only known bacterium capable of thriving in the harsh, acidic environment of the human gastric mucosa. In 1983, scientists Barry J. Marshall and Robin Warren identified this bacterium for the first time from biopsy samples of patients with chronic gastritis, an achievement that later earned them the Nobel Prize in Physiology or Medicine in 2005.
H. pylori’s Secret Defense Mechanism
The key to H. pylori’s survival in the acidic stomach lies in its ability to produce urease, an enzyme that converts urea in the stomach into carbon dioxide and ammonium, effectively neutralizing the surrounding acid. In essence, H. pylori carries its own miniature “shield” that allows it to cleverly persist in the gastric acids.
H. pylori and Its Role in Gastric Diseases: An Internal Saboteur
Infection with H. pylori is considered a leading culprit behind various gastric diseases:
Peptic Ulcers: Imagine your stomach wall being eroded by tiny bacteria, creating painful cavities—these are ulcers.
Chronic Gastritis: Long-term cohabitation with H. pylori may lead to inflammation of the gastric mucosa, eventually evolving into chronic gastritis.
Gastric Cancer: In severe cases, this persistent inflammation can increase the risk of developing gastric cancer.
Transmission Routes of H. pylori
- Oral-oral Transmission: H. pylori can survive in the oral cavity and proliferate on dental plaque and carious teeth. Direct contact through sharing utensils, cups, and cutlery can transfer the bacteria from person to person via saliva. Kissing is also a direct form of oral-oral contact that can spread H. pylori. Parents feeding children by chewing food, mouth-to-mouth feeding, or kissing infants on the lips can also lead to transmission.
- Fecal-oral Transmission: H. pylori present in an infected person’s feces can contaminate food or water sources, especially if these are not thoroughly cooked or disinfected, potentially infecting those who consume them.
- Poor hygiene practices, such as not washing hands before eating or after using the toilet, can indirectly lead to fecal-oral transmission.
- Vomiting Transmission: When an infected person vomits or experiences gastroesophageal reflux, vomitus containing H. pylori can contaminate the surrounding environment and subsequently enter another person’s mouth through food or drink.
- Mother-to-child Transmission: This includes exposure during childbirth to the mother’s vaginal secretions, contact with an infected mother’s nipple during breastfeeding, and improper feeding methods (such as mouth-to-mouth feeding or feeding children after chewing food).
- Waterborne Transmission: H. pylori can exist in the external environment under certain conditions, such as water sources. Drinking contaminated water can trigger infection.
- Iatrogenic Transmission: Within medical settings, if disinfection procedures are not strictly followed, medical instruments like endoscopes and dental tools can become vectors for transmission.
To effectively prevent H. pylori infection, emphasis should be placed on improving personal hygiene habits, implementing separate dining practices, ensuring food safety and drinking water hygiene, enhancing disinfection and sterilization in medical environments, and screening and treating high-risk populations.
What Symptoms Appear After Infection?
Symptoms of H. pylori infection vary from person to person, and some individuals may not exhibit any noticeable symptoms. However, common potential symptoms include:
- Abdominal Discomfort: Many people experience abdominal discomfort or upper abdominal pain following H. pylori infection. This pain typically occurs after meals or at night and may fluctuate in intensity.
- Digestive Issues: H. pylori infection can cause digestive problems such as heartburn, bloating, acid reflux, etc. Some may also experience belching, nausea, vomiting, or diarrhea.
- Reduced Appetite: H. pylori infection may affect appetite, leading to reduced desire to eat or weight loss.
- Nausea and Vomiting: In some cases, H. pylori infection may cause nausea and vomiting, often occurring when complications like gastric ulcers or gastritis arise.
- Anemia: Long-term H. pylori infection can damage the gastric mucosa, affecting the absorption of nutrients like iron and vitamin B12, which can lead to anemia.
Not everyone infected with H. pylori will exhibit these symptoms. Some may have no symptoms or only mild discomfort but still carry the bacteria. If you suspect you might be infected with H. pylori, consult a doctor for diagnosis and treatment recommendations.
Detecting the “Invisible” Enemy: Testing for H. pylori
Fortunately, modern medicine has developed various methods to detect H. pylori:
Breath Test: Simple, painless, and highly effective, it determines infection by measuring specific marker molecules in your breath.
Blood Test: Checks for antibodies against H. pylori in your blood.
Endoscopy Sampling Test: Directly samples the gastric mucosa for laboratory culture, yielding highly accurate results.
Evicting H. pylori: The Key to Victory in the Battle Against Stomach Diseases
If test results are positive, don’t worry! Doctors usually employ a “triple therapy” approach to combat these unwelcome bacteria:
Two Antibiotics: Used simultaneously to reduce the chance of bacterial resistance.
Proton Pump Inhibitor: Reduces stomach acid secretion, providing an environment for the gastric mucosa to heal.
This treatment combination typically lasts 7 to 14 days and has a success rate of over 90%!
How to Prevent H. pylori Infection?
- Good Personal Hygiene: Maintaining good personal hygiene, such as frequent handwashing and using clean restroom and kitchen facilities, can reduce the chances of bacterial transmission.
- Food Hygiene: Ensure the safety of food and water sources by avoiding raw or undercooked foods, especially seafood and meats. Also, pay attention to food storage and handling to prevent cross-contamination.
- Avoid Close Contact with Infected Individuals: H. pylori can spread through saliva, feces, and other means, so avoid intimate contact with infected persons, such as sharing utensils and cups.
- Limit Antibiotic Use: Misuse of antibiotics can disrupt the stomach’s microbial balance, increasing the risk of H. pylori infection. Use antibiotics only under medical guidance and rationally.
- Environmental Hygiene: Keep living areas clean and hygienic, especially bathrooms and kitchens, which are prone to contamination.
- Regular Health Checkups: Regularly undergo gastrointestinal-related checkups, such as endoscopies, as well as tests for H. pylori.
While these measures can lower the risk of H. pylori infection, they cannot eliminate it entirely. If you suspect you have been infected with H. pylori, seek medical advice for diagnosis and treatment options.
Understanding and paying attention to H. pylori is crucial for maintaining our gastric health. Early detection, prompt treatment, and prevention through lifestyle changes can effectively fend off this “gastric devil,” making health a norm in our daily lives. Remember to schedule regular checkups to stay informed about your health status and truly prevent problems before they arise, ensuring a healthy life every day.