Alcohol, a widely consumed substance globally, is often associated with social interactions and relaxation for many. However, excessive alcohol consumption is linked to various health issues, particularly liver damage that should not be overlooked. Such damage can lead to chronic conditions like alcoholic liver disease and may even progress to liver cancer.

Alcoholic Liver Disease: The Hidden “Killer”
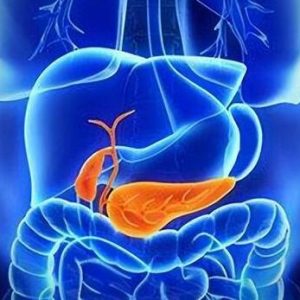
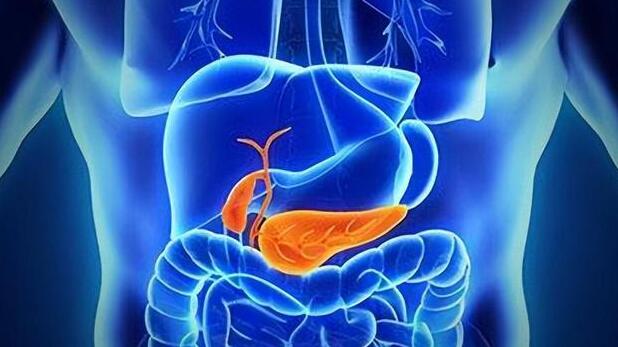
Alcoholic liver disease results from long-term heavy drinking, causing the liver to break down alcohol into acetaldehyde, which can harm liver cells and lead to progressive liver dysfunction. Initially, there may be no apparent symptoms, but as the condition worsens, individuals may experience fatigue, loss of appetite, jaundice, and other symptoms.
Stages of Alcoholic Liver Disease to Liver Cancer
- 1. Alcoholic Fatty Liver: This initial stage involves fat accumulation in the liver due to long-term excessive drinking and is usually reversible without significant symptoms.
- 2. Alcoholic Hepatitis: Prolonged alcohol abuse can trigger inflammation, known as alcoholic hepatitis, which may present with jaundice and abdominal pain. It can be reversible, but continued drinking may lead to more severe liver damage.
- 3. Alcoholic Cirrhosis: Uncontrolled alcoholic hepatitis leads to permanent changes in liver structure and function, manifesting as cirrhosis with symptoms like ascites and gastrointestinal bleeding, which is irreversible.
- 4. Liver Cancer: Cirrhosis patients have an increased risk of developing hepatocellular carcinoma (HCC). While alcoholic cirrhosis elevates the risk of liver cancer, not all cirrhosis patients will develop it; it’s a risk factor influenced by genetics, viral hepatitis infections (like B and C), exposure to certain chemicals or medications.
Not everyone will go through these stages sequentially; individual circumstances vary. Additionally, the development of liver cancer can be influenced by factors beyond alcoholic liver disease.
Warning Signs of Alcoholic Liver Disease
- – Digestive symptoms: decreased appetite, nausea, vomiting, abdominal pain (especially in the upper right)
- – Body changes: weight loss, abdominal swelling (potentially from ascites)
- – Skin and eye changes: jaundice, skin itching
- – Mental and behavioral changes: irritability, mood swings, confusion, or lethargy (which can progress to hepatic encephalopathy)
- – Other symptoms: black or bloody stools (indicating internal bleeding), fatigue, muscle wasting
These symptoms can indicate liver problems and reflect the extent of liver damage. Seeking medical attention promptly and considering abstinence from alcohol can prevent further liver injury.
Treatment for Alcoholic Liver Disease
1. Abstinence: The most crucial step in treating alcoholic liver disease. Even after liver damage has occurred, stopping alcohol consumption can prevent further deterioration and may help in partial liver repair.
2. Nutritional support: Alcohol-dependent individuals often suffer from malnutrition, so improving dietary habits to ensure adequate protein, vitamins, and nutrients is beneficial.
3. Medication: In some cases, drugs may be used to reduce inflammation, treat complications, or aid liver repair, such as corticosteroids for alcoholic hepatitis or antioxidants like vitamin E and S-adenosylmethionine (SAMe).
4. Monitoring and managing complications: Alcoholic liver disease can cause portal hypertension, ascites, hepatic encephalopathy, etc., requiring targeted treatments.
5. Psychosocial support: Quitting alcohol is a long process that might require psychological support and counseling.
6. Liver transplantation: In extreme cases where liver function cannot be restored through medication, a liver transplant may be considered.
Any treatment plan should be under medical supervision, with individualized approaches based on specific circumstances.
How to Reduce Risk in Daily Life?
1. Limit alcohol consumption: The most direct and effective method is to reduce or stop drinking.
2. Healthy diet: A balanced diet contributes to good liver health, including plenty of fruits, vegetables, whole grains, and limiting high-calorie foods, saturated fats, and refined sugars. Consider incorporating olive oil, deep-sea fish, and nuts for liver benefits.
3. Maintain a healthy weight: Obesity increases the risk of non-alcoholic fatty liver disease, leading to liver damage. Control weight through proper diet and regular exercise.
4. Regular exercise: Physical activity helps manage weight and lower the risk of liver disease. Aim for at least 150 minutes of moderate-intensity exercise weekly.
5. Avoid toxic substances: Minimize exposure to industrial chemicals and tobacco smoke, which can exacerbate liver damage.
6. Careful with medication use: Some drugs (including over-the-counter) can stress the liver if used with alcohol. Follow doctor’s advice when taking any medication.
7. Prevent infections: Protect yourself from viruses that cause hepatitis, such as hepatitis B and C. Avoid direct contact with others’ blood or bodily fluids, do not use unsterilized needles, and consider hepatitis B vaccination.
8. Monitor liver health: Regularly check liver function, especially if you drink or have other risk factors for liver disease.
9. Good personal hygiene: Wash hands frequently, especially after handling food or using the restroom.
10. Sensible use of supplements and herbal products: Some can have side effects on the liver, especially in large doses or long-term use. Always inform your doctor about all products used and follow professional advice.
By adopting these measures, one can significantly reduce the risk of liver damage due to alcohol consumption and promote overall health. If you have liver disease, it’s best to manage your condition under the guidance of healthcare professionals.