Blood, the river of life flowing within our bodies, carries with it the essence of vitality. However, when the “fats” in this river become excessive, they silently brew a hidden danger to health – hyperlipidemia. This condition, much like an invisible assassin, stealthily erodes the well-being of our cardiovascular system.
What is Hyperlipidemia?
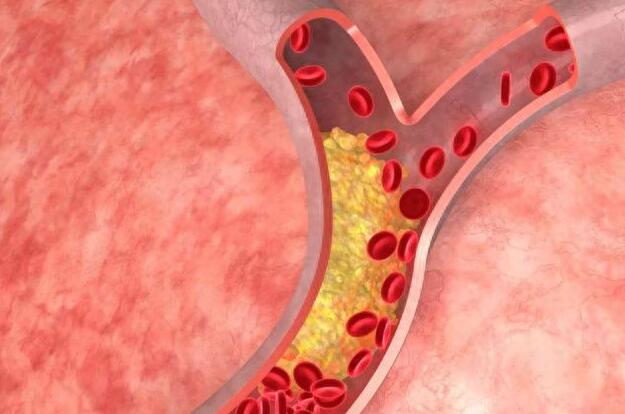
Hyperlipidemia, as the name suggests, refers to a state where the lipid content in the blood, primarily cholesterol and triglycerides, is abnormally high. When these substances exceed normal levels, they gradually accumulate on the walls of blood vessels, forming plaques that lead to arteriosclerosis, which can ultimately result in life-threatening cardiovascular events such as heart attacks and strokes.
Why Should You Be Wary of It?
Many people may dismiss hyperlipidemia as a distant concern, but in reality, it’s becoming increasingly common and deceptively cunning. With few overt symptoms, it’s often only detectable through blood tests. Those with long-term hyperlipidemia have a significantly higher incidence of cardiovascular diseases compared to the general population, earning it the moniker “the silent health killer.”
How Do You Know If You Have Hyperlipidemia?
The greatest challenge with hyperlipidemia is its silence. Most people don’t experience any discomfort in the early stages of the disease. Over time, symptoms such as fatigue, dizziness, and memory decline may appear. In more severe cases, it can cause chest tightness, pain, and other heart-related symptoms, or precursors to a stroke.
The most direct way to confirm hyperlipidemia is through a blood lipid test. It’s generally recommended that adults undergo this test at least once a year, especially those with risk factors like family history, obesity, or poor lifestyle habits.
How to Prevent and Treat Hyperlipidemia?
Balanced Diet:
- Adopt the “four lows and one high” dietary principle: low-calorie, low-fat, low-cholesterol, low-sugar, and high-fiber diet.
- Reduce intake of saturated and trans fats found in animal fats, fatty meats, cream, butter, and some processed foods.
- Control total calorie intake, particularly for those who are overweight or obese, reducing daily intake to appropriate levels.
- Prefer oils rich in unsaturated fats like olive oil and peanut oil.
- Increase consumption of vegetables, fruits, whole grains, legumes, and nuts, which are rich in dietary fiber and beneficial nutrients.
- Limit salt intake to prevent hypertension and edema.
2. Weight Management:
- For those overweight or obese, achieve energy deficit through dietary adjustments and increased physical activity to reduce weight.
- Maintain an ideal Body Mass Index (BMI), generally between 18.5-23.9 kg/m².
3. Lifestyle:
- Engage in regular, structured physical exercise, such as at least 150 minutes of moderate-intensity aerobic activities per week, like jogging, swimming, or cycling.
- Quit smoking and limit alcohol consumption; tobacco harms lipid metabolism, and moderate drinking can raise triglyceride levels, with excessive drinking leading to fatty liver.
- Maintain good sleep patterns, reduce stress, and keep an optimistic mindset.
4. Regular Monitoring:
- Perform regular lipid profile checks, especially for high-risk groups such as those over 40, with a family history, or with chronic conditions like hypertension or diabetes.
5. Medication:
- When lifestyle interventions fail to lower lipid levels effectively, medication under a doctor’s guidance may be necessary. Common drugs include agents that lower triglycerides, like fibrates (e.g., fenofibrate, bezafibrate); cholesterol-lowering statins (e.g., simvastatin, rosuvastatin, atorvastatin); and for specific types of hyperlipidemia, additional drugs like ezetimibe or PCSK9 inhibitors may be used.
Combating hyperlipidemia requires an individualized approach. Implement strategies under professional medical guidance, persist with long-term management and self-monitoring, and cultivate healthy living habits to help prevent and manage hyperlipidemia and its complications.