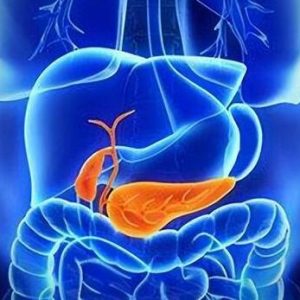
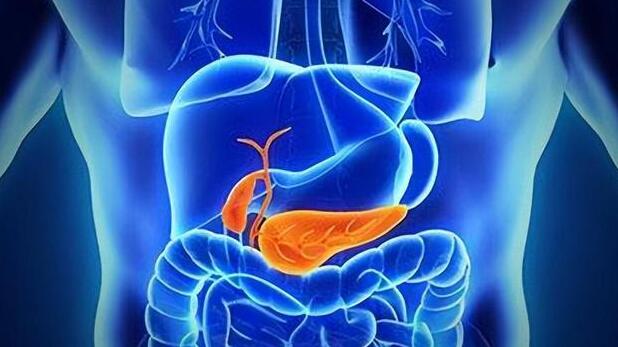
The pancreas, located deep within the abdomen, plays a pivotal role in our body, albeit not as conspicuously as some other organs. It is responsible for producing digestive enzymes that break down food and hormones like insulin to regulate blood sugar levels. However, when inflammation occurs in this unassuming organ, it’s known as pancreatitis.

Types of Pancreatitis
There are generally two types of pancreatitis:
1. Acute Pancreatitis: This is a sudden onset of inflammation that can lead to abdominal pain, nausea, and vomiting. While most people recover fully, it can sometimes become severe and even life-threatening.
2. Chronic Pancreatitis: The result of long-term inflammation, it can cause permanent damage to the pancreas. This form of pancreatitis can lead to digestive issues and diabetes.
Causes of Pancreatitis
The reasons behind pancreatitis can vary:
1. Gallstones: These can block the opening shared with the pancreas (the Sphincter of Oddi), leading to the buildup of pancreatic fluid and inflammation.
2. Alcohol Abuse: Long-term alcohol consumption can lead to bouts of chronic pancreatitis.
3. Hypertriglyceridemia: Exceptionally high levels of triglycerides can trigger pancreatitis.
4. Medications: Certain drugs, such as diuretics, immunosuppressants, and some HIV treatments, may cause pancreatitis.
5. Infections: Viral (like the mumps virus, cytomegalovirus) or bacterial infections can also lead to pancreatitis.
6. Genetic Factors: A family history of pancreatitis might indicate a genetic predisposition.
7. Autoimmune Disorders: Autoimmune pancreatitis occurs when the immune system mistakenly attacks and damages pancreatic tissue.
8. Trauma or Surgery: Pancreatitis can occur post-abdominal trauma or after pancreatic surgery.
9. Endoscopic Retrograde Cholangiopancreatography (ERCP): This medical procedure to examine the bile and pancreatic ducts can sometimes induce pancreatitis.
10. Metabolic Diseases: For example, hypercalcemia.
Typically, pancreatitis is divided into acute and chronic forms. Acute pancreatitis has a sudden onset, can fully recover, but may also become severe with life-threatening risks. Chronic pancreatitis is a persistent, chronic inflammation process that may lead to permanent pancreatic damage over time.
Symptoms of Pancreatitis
Symptoms of pancreatitis vary among individuals but commonly include:
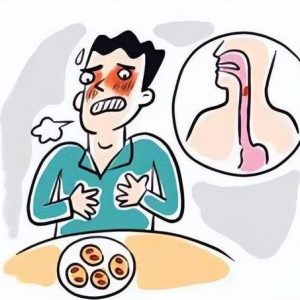
1. Abdominal Pain: Located in the upper left abdomen or throughout the abdomen, the pain is intense and can radiate to the back.
2. Nausea and Vomiting: Frequent vomiting, possibly containing food or bile.
3. Fever: Some patients with pancreatitis may exhibit fever symptoms.
4. Jaundice: Due to biliary obstruction, jaundice may occur.
When the pancreas is inflamed, it may not be able to produce or secrete digestive enzymes effectively. This means foods, especially fats and proteins, cannot be normally digested and absorbed. Therefore, adjusting dietary habits is essential to reduce the pancreas’s workload.
Basic Principles of Dietary Adjustment
– Low-fat Diet: High-fat foods increase the burden on the pancreas, so opting for low-fat options is advisable.
– Small, Frequent Meals: Avoid large meals as they increase the demand for digestive enzymes from the pancreas.
– Avoid Alcohol: A common cause of pancreatitis, abstaining from alcohol is crucial for prevention and control.
– Adequate Hydration: Staying hydrated helps alleviate metabolic stress and support normal bodily functions.
Recommended Food Choices
– Whole Grains and High Fiber Foods: Like oatmeal, brown rice, and whole wheat bread, but be mindful not to overconsume fiber to avoid extra digestive load.
– Lean Proteins: Such as chicken, turkey, and fish, skinless and deboned to provide necessary protein while reducing fat intake.
– Fruits and Vegetables: Fresh produce packed with vitamins and minerals aids in overall body recovery.
– Low-fat Dairy Products: Options like skim milk or low-fat yogurt meet calcium needs without excessive fat.
Foods to Avoid
– Fried Foods and Fast Foods: Often high in fats, these stimulate more digestive enzyme production from the pancreas.
– High-fat Meats: Such as pork, lamb, and meats with abundant subcutaneous fat.
– Sugary Drinks and Desserts: These can cause a rapid increase in blood sugar, adding extra pressure on the pancreas.
– Processed and Canned Foods: Often high in salt, sugar, and/or fat.
Practical Dietary Management Strategies
– Food Journal: Record your diet to help identify potential discomfort-triggering foods.
– Regular Mealtimes: Consistent eating times help maintain digestive system stability.
– Consult a Dietitian: Professional nutritionists can offer personalized dietary advice based on your specific situation.
Dietary management for those with pancreatitis is an ongoing process requiring collaboration between patients, their families, and the medical team. With dietary adjustments combined with doctor guidance and medication, patients can effectively manage their condition and enhance their quality of life. Healthy eating is not just part of treatment but a lifestyle change.
Treatment for Pancreatitis
Acute Pancreatitis
1. Rest the Pancreas: Temporarily stop eating and provide intravenous nutrition to reduce the pancreas’s workload.
Severe cases may require nasogastric tube suction to remove stomach contents.
2. Pain Relief: Use NSAIDs or opioid medications to alleviate pain.
3. Fluid and Electrolyte Replacement: Maintain body hydration and electrolyte balance through IV fluids.
4. Nutritional Support: Gradually reintroduce feeding once symptoms subside, starting with clear liquid diets before transitioning to low-fat solid foods. Sometimes feeding through a nasojejunal or gastrostomy tube is necessary.
5. Antibiotics: If infection is present, antibiotics may be needed.
6. Surgery or Other Procedures: To remove peripancreatic fluid collections or necrotic tissue. To address biliary issues or remove gallstones.
Chronic Pancreatitis
1. Pain Management: Through NSAIDs, opioid analgesics, nerve blocks, etc.
2. Enzyme Replacement Therapy: Oral pancreatic enzymes to aid digestion and reduce diarrhea and weight loss.
3. Quit Smoking and Alcohol: Eliminate triggers, especially avoiding alcohol.
4. Dietary Adjustments: Follow a low-fat diet, consume more carbohydrates, and less high-fat food.
5. Treat Complications: Such as diabetes or malabsorption.
6. Endoscopic or Surgical Interventions: To decompress pancreatic ducts, remove necrotic tissue, or cancerous areas.
7. Manage Metabolic Complications: Like diabetes caused by exocrine pancreatic insufficiency.
Precautions
The exact treatment plan for pancreatitis should be determined by a doctor based on the patient’s specific circumstances. Patients should adhere to medical advice, undergo regular check-ups, eat sensibly, and manage themselves under professional medical guidance. All medical advice should be sought directly with a doctor; the information above does not replace professional medical opinion. If you or someone you know exhibits symptoms of pancreatitis, seek medical attention promptly.