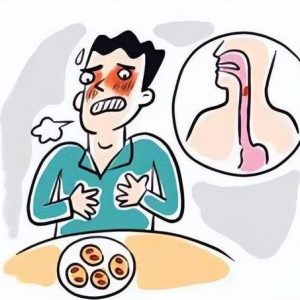
Angina, a term that resonates with discomfort, serves as a critical warning signal from our heart. It represents a transient ischemic and hypoxic state of the heart muscle, caused by insufficient coronary artery blood supply, demanding our utmost attention and immediate action.
What does Angina feel like?
This is not merely a simple chest discomfort; it’s a cry for help from the heart. Patients often describe an overwhelming sensation of chest compression, heaviness, pain, or even a burning feeling, as if an elephant were sitting on their chest or a pair of pliers tightly clamping their heart.
Why does Angina occur?
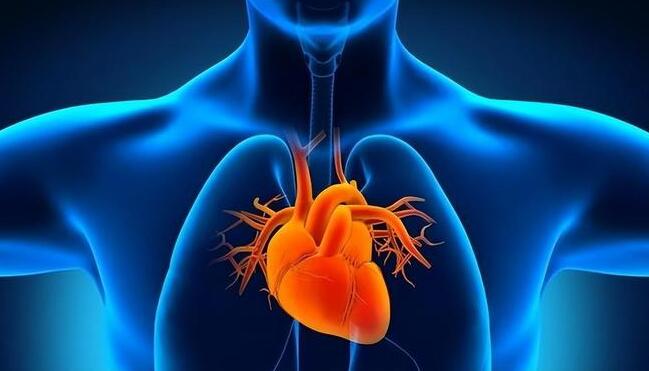
The culprit behind Angina is Coronary Artery Disease (CAD). The coronary arteries are the vessels that cover the heart, responsible for delivering oxygen and nutrients to the cardiac muscle. When these arteries become narrow due to plaque buildup, the heart’s blood supply becomes inadequate, particularly during brisk walking, climbing stairs, or emotional stress.
Types of Angina
- Stable Angina: This type typically occurs during certain activities, is predictable, and can be relieved by rest and/or nitroglycerin.
- Unstable Angina: A more alarming sign indicating the coronary artery may soon become completely blocked. The pain can occur at rest, is unpredictable, and may increase in frequency, intensity, and duration.
- Variant (Prinzmetal) Angina: Rarely, this type occurs at rest due to temporary spasms in the coronary artery.
Signals of Angina
Besides chest pain, Angina may accompany other symptoms, including but not limited to:
- Chest discomfort
- Shortness of breath
- Nausea
- Abnormal sweating
- Dizziness or lightheadedness
- Fatigue
- Pain in the jaw, neck, back, or arms
How is Angina diagnosed?
- 8. Detailed history collection: Inquiring about the nature, onset time, duration, triggers, radiation areas, and relieving factors of symptoms.
- 9. Physical examination: Assessing vital signs (such as blood pressure and heart rate), listening for any abnormal heart or respiratory sounds.
- 10. Electrocardiogram (ECG): ECG detects electrical activity of the heart, looking for signs of ischemia or previous myocardial infarction.
- 11. Blood tests: Measuring levels of cardiac injury markers (like troponins), which rise when the heart is damaged.
- 12. Stress test (Exercise ECG): Monitoring ECG, heart rate, and blood pressure changes while the patient exercises on a treadmill or bicycle to assess the heart’s response to increased workload.
- 13. Imaging studies: Such as coronary angiography, using X-ray imaging to view the condition of the coronary arteries.
- 14. Cardiac ultrasound (Echocardiogram) to assess ventricular wall motion and overall heart function.
- 15. Nuclear medicine cardiac scans (like myocardial perfusion imaging) to evaluate the blood supply to the heart muscle under rest and stress conditions.
- 16. Computed Tomography (CT): Coronary CT can assess the degree of calcification and the location and extent of narrowing of the coronary arteries.
- 17. Magnetic Resonance Imaging (MRI): Cardiac MRI provides detailed information about heart structure and function and can also help diagnose certain types of Angina.
- 18. Invasive diagnostic tests: Coronary angiography is the gold standard, directly observing coronary artery blood flow and obstructive lesions.
These tests are often used in combination to ensure accurate diagnosis of Angina and its causes. Doctors will decide which specific tests are needed based on initial results and the patient’s personal risk factors.
So, what should we do?
If you experience the above symptoms, seek medical help immediately. Treatment for Angina includes:
- Medication: Doctors may prescribe drugs to alleviate symptoms and prevent cardiac events, such as nitrates (like nitroglycerin), calcium channel blockers, β-blockers, and anticoagulants.
- Revascularization (Interventional treatment): A non-surgical method using catheters inserted through the blood vessels to expand narrowed coronary arteries, restoring blood flow. This includes Percutaneous Coronary Intervention (PCI) and Coronary Artery Bypass Grafting (CABG).
- Lifestyle improvement: Changing lifestyle can help improve symptoms and prevent the progression of heart disease. This includes quitting smoking, adopting a healthy diet, moderate exercise, controlling weight, reducing stress, and limiting alcohol intake.
- Psychological support: Angina may affect patients’ mental health, so receiving psychological support and counseling is also an important aspect of treatment. These are general suggestions. Each person’s situation is different, and treatment should be based on individualized medical advice and guidance. If you or someone else shows symptoms of Angina, seek professional medical opinion immediately.
Prevention is always better than cure
The best “therapy” for Angina might be preventing its occurrence.
- Healthy diet: Adopt a balanced diet rich in fresh fruits, vegetables, whole grains, and healthy fats (like olive oil, fish oil), while limiting high-salt, high-cholesterol, and high-saturated-fat foods.
- Physical exercise: Engage in moderate aerobic activities like brisk walking, swimming, or cycling, for at least 150 minutes weekly. Consult a doctor before starting any new exercise program.
- Maintain a healthy weight: Keeping an appropriate weight is very important for heart health. If overweight or obese, reduce weight through a sensible diet and exercise.
- Quit smoking: Smoking greatly harms heart health, so it’s best to quit or avoid secondhand smoke exposure.
- Control blood pressure and cholesterol: Keeping blood pressure and cholesterol levels within normal ranges can reduce the risk of heart disease. Follow your doctor’s advice for treatment and control if you have high blood pressure or cholesterol issues.
- Control diabetes: For those with diabetes, maintaining good blood sugar control is crucial. Follow your doctor’s advice for treatment and management.
- Reduce stress: Find appropriate ways to cope with stress, such as relaxation techniques, meditation, and exercise, to lessen the impact of psychological stress on heart health.
- Regular check-ups: Regular physical exams and checks, including monitoring blood pressure, cholesterol, glucose, and other indicators, can help detect and control potential heart disease risk factors early on. These are general methods to prevent Angina. Each person’s situation is different, so it’s best to develop a personalized prevention plan based on your medical history and doctor’s advice.
Angina, though painful to the heart, serves as an alarm bell, reminding us to care for our heart health. Through scientific lifestyle adjustments, strict disease management, proactive psychological adaptation, and regular health check-ups, we can effectively reduce the risk of Angina and protect the engine of life – our heart.