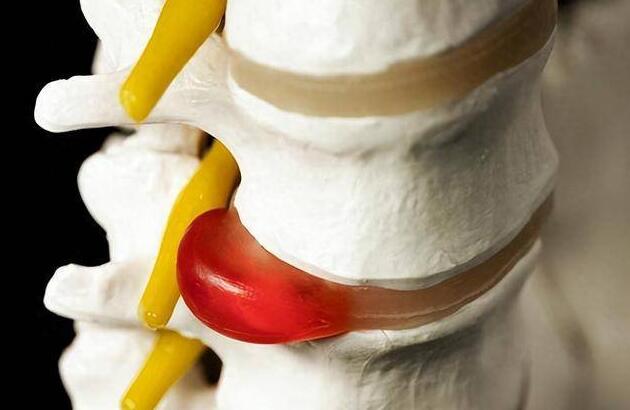
Lumbar disc herniation, also known as a slipped or bulging disc, can be likened to a jelly-filled biscuit in your spine that unexpectedly oozes its filling. The intervertebral discs in our spine serve as cushions between the vertebrae, and when the gel-like substance in the center, known as the nucleus pulposus, is pushed beyond the outer fibrous ring due to force or degeneration, pain becomes an unwelcome guest.
Why Does It Happen?
The reasons for lumbar disc herniation can vary:
- Aging: As time goes by, our discs lose hydration, becoming less elastic and more susceptible to injury.
- Lifestyle Factors: Prolonged poor sitting posture, frequent heavy lifting, and being overweight are continuous “micro-injuries” to the discs.
- Genetic Predisposition: If someone in your family has had this issue, your risk may be relatively higher.
- Traumatic Events: Sudden injuries from car accidents or falls can lead to direct damage of the discs.
What Are the Symptoms?
Lumbar disc herniation may cause one or several of the following symptoms:
- Back Pain: This is one of the most common symptoms, ranging from mild discomfort to severe pain, which can worsen with changes in posture, such as bending or standing.
- Sciatica: When the protruding disc compresses a nearby nerve root, it can cause shooting pain along the nerve’s path, typically down one side of the lower back or outer leg, sometimes extending to the foot.
- Numbness or Tingling: These sensations usually occur along the nerve’s distribution in the lower limbs.
- Muscle Weakness: The affected nerve root may cause weakness in the muscles of the thigh, calf, or foot.
- Diminished Reflexes: Nerve damage can lead to weakened knee or ankle reflexes.
- Walking Difficulties: Pain and muscle weakness can affect ambulation, making it difficult for patients to stand or walk.
- Postural Changes: To alleviate pain, patients might unconsciously alter their standing or walking postures. In severe cases, disc herniation can affect the cauda equina nerves, leading to a medical emergency known as cauda equina syndrome, with symptoms including bilateral leg pain, severe numbness or leg weakness, and difficulty urinating or defecating. Seek immediate medical attention if these symptoms occur.
Symptom severity does not always correlate with the size of the disc herniation; some people with significant protrusions may be asymptomatic, while others with smaller protrusions can experience severe symptoms.
What Should I Do?
First, relax and take a deep breath. Modern medicine is increasingly humane and precise in addressing lumbar disc herniation.
- Conservative Treatment: Physical therapy, medication, and injection therapy are common initial strategies. With professional guidance, you can allow the damaged disc to rest and recover.
- Daily Exercise: Activities like swimming and yoga can strengthen core muscles, stabilize the spine, and reduce future risks.
- Physical Medicine Specialist: They can create a personalized rehabilitation plan based on your condition.
- Surgery: If symptoms are severe or conservative treatment is ineffective over time, minimally invasive surgery can be an option to remove the compressed nerve tissue, restoring freedom.
How Can Patients Manage Their Condition Daily?
- Rest and Postural Adjustment: During the acute phase, patients should rest in bed, ideally lying flat for 2 to 3 weeks on a firm mattress to prevent increased lumbar curvature. Use axial rolling to change positions without twisting the lower back. Gradually increase activity with a lumbar support belt after stabilization and avoid prolonged standing or sitting.
- Exercise and Rehabilitation Training: After recovery or symptom relief, appropriate rehabilitation exercises should begin, such as strengthening the lower back muscles with exercises like “little sparrow flying,” three-point support, and five-point support to enhance lumbar stability. Avoid high-intensity activities or those that could increase lumbar load, like bending to lift heavy objects or twisting the lower back vigorously.
- Lifestyle Adjustments: Keep warm to avoid cold aggravating symptoms. Maintain a healthy weight; excess weight adds pressure to the spine. Avoid long periods of fixed posture; get up and move around regularly to improve circulation. Quit smoking and limit alcohol consumption; both can affect blood flow and bone health.
- Medication Management and Treatment Compliance: Take medications correctly as prescribed by your doctor, such as nonsteroidal anti-inflammatory drugs (NSAIDs), muscle relaxants, or painkillers, usually taken half an hour after meals to reduce gastrointestinal irritation. Follow medical advice after physical therapy or spinal injections, such as lying quietly for a certain time after injections.
- Dietary Regulation: Eat a balanced diet rich in protein, calcium, and vitamin D, found in eggs, milk, fish, and green vegetables, to support bone health. Reduce spicy foods to prevent constipation; eat fiber-rich fruits and vegetables to keep bowel movements smooth and reduce lumbar pressure during defecation.
- Psychological Care: Provide necessary psychological support; encourage patients to stay optimistic, recognizing that the disease is treatable and can recover, avoiding the impact of mental stress on recovery.
Under the professional guidance of the medical team, patients can better manage lumbar disc herniation, accelerate the recovery process, and reduce the risk of recurrence. Additionally, regular follow-ups and returning for medical appointments as advised are essential parts of the process.
Lumbar disc herniation may seem like a betrayal by our bodies, but it’s actually a reflection of our lifestyle choices. Although it’s a common health issue, understanding, preventing, and scientifically treating it can effectively alleviate symptoms and restore lumbar health. Let’s start now by focusing on our spinal health and steering clear of the troubles caused by lumbar disc herniation!