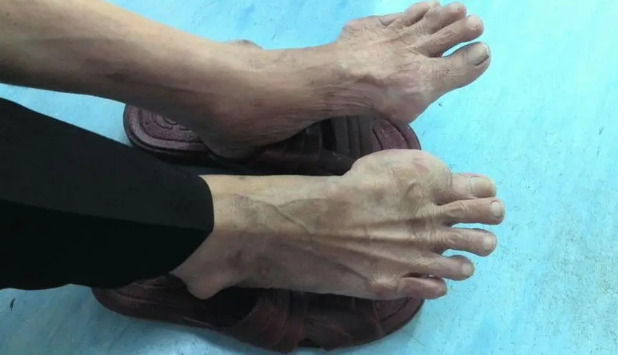
Gout is clinically characterized as a type of metabolic arthritis, primarily caused by the deposition of uric acid in the joint cavity, which triggers an inflammatory response leading to symptoms such as joint pain, swelling, or deformity.
When not in an acute flare-up, one might forget its presence; however, once it strikes, the pain can be unbearable.
This article introduces three major classes of medications used in the treatment of gout.
1. Analgesic Drugs
– Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): These are the drugs of choice for gout. NSAIDs are divided into selective COX-2 inhibitors (such as celecoxib, etoricoxib, etodolac, and meloxicam) and non-selective COX inhibitors (such as diclofenac sodium, ibuprofen, NIMESULide, and loxoprofen sodium). Compared to non-selective COX inhibitors, selective COX-2 inhibitors have a smaller impact on gastrointestinal mucosa but carry a greater risk to the cardiovascular system.
– Colchicine: It is also a frontline treatment for acute gout flares. Due to the narrow therapeutic window of colchicine, overdosing can easily lead to toxic reactions. Moreover, there is no significant difference in the effectiveness of treating gout between low and high doses of colchicine. Therefore, current guidelines both domestically and internationally recommend using low-dose colchicine to significantly reduce adverse reactions. However, common side effects of colchicine include diarrhea, abdominal pain, and nausea. If severe diarrhea occurs, discontinuation is necessary, and potential liver and kidney damage as well as bone marrow suppression should be monitored regularly through liver and kidney function tests and blood counts. During the urate-lowering treatment period, to prevent acute gout flares,
2. Urate-Lowering Drugs
– Inhibitors of Uric Acid Production
Allopurinol and febuxostat are both drugs that inhibit uric acid production. Compared to allopurinol, febuxostat has advantages in three main aspects: stronger urate-lowering effect, higher safety, and rare occurrence of allergic reactions; it can be excreted through both liver and kidney pathways, making it suitable for patients with liver or kidney dysfunction.
One disadvantage of febuxostat is the increased risk of cardiovascular events with long-term use, so patients with congestive heart failure need to weigh the pros and cons. Conversely, allopurinol can improve endothelial function and local blood flow in patients with heart failure accompanied by hyperuricemia, indicating that allopurinol can provide additional cardiovascular protection.
Both allopurinol and febuxostat have renal protective effects, hence they are preferred overbenzbromarone for patients with renal insufficiency.
– Enhancers of Uric Acid Excretion
Benzbromarone belongs to the class of drugs that promote uric acid excretion. By inhibiting the reabsorption of uric acid and enhancing its excretion, it reduces serum uric acid levels. Therefore, benzbromarone is recommended for patients with poor uric acid excretion. Research indicates that most hyperuricemic individuals in China have poor uric acid excretion, making benzbromarone potentially more suitable for the Chinese population.
The severe adverse reaction of benzbromarone is hepatotoxicity, which increases when used in combination with other drugs such as allopurinol, simvastatin, atorvastatin, and leflunomide. In 2004, the National Medical Products Administration warned about the risk of liver damage from benzbromarone. Benzbromarone can also increase the incidence of urinary stones. It is contraindicated in patients with urinary stones or moderate renal insufficiency. During treatment, it is necessary to drink plenty of water to increase urine output or to alkalinize the urine to prevent the formation of uric acid crystals.
3. Drugs for Alkalinizing Urine
– Sodium Bicarbonate Tablets: These are commonly used clinically to alkalinize urine. Since sodium bicarbonate produces carbon dioxide in the stomach, increasing the intragastric pressure, long-term and excessive use can lead to alkalosis and may induce congestive heart failure and edema due to increased sodium load. When uric acid is acidic in the morning, acetazolamide can be taken at night to increase uric acid solubility and prevent stone formation.
– Potassium Citrate Hydrogen Salt Granules: These are used to alkalinize urine and should not be used in patients with acute or chronic renal failure, or in those with severe acid-base imbalances (alkalosis) or chronic urease-splitting bacterial infections in the urinary tract.
Note: Gout patients should avoid long-term use of medications that may cause elevated blood uric acid levels, such as thiazide diuretics, loop diuretics, low-dose aspirin, tacrolimus, cyclosporine, pyrazinamide, ethambutol, methotrexate, insulin, etc.
Gout patients should actively treat metabolic and cardiovascular risk factors associated with elevated blood uric acid levels, and actively control obesity, type 2 diabetes, hypertension, hyperlipidemia, coronary heart disease, stroke, or chronic kidney disease. Metformin, dapagliflozin, atorvastatin, fenofibrate, losartan, etc., while lowering blood sugar, lipids, and blood pressure, all have varying degrees of urate-lowering effects and can be given priority.